‘Melton vaccine centre is a beacon of hope for a brighter future’
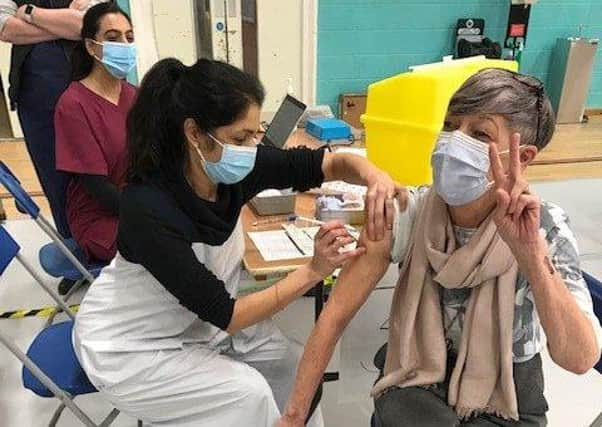

More than 12,500 people had received their first of two doses of the vaccine at Melton Sports Village by last week, with all priority cases - those aged over 70, the clinically extremely vulnerable and frontline health and care workers - having already been offered a jab.
We spoke to Dr Fahreen Dhanji, a GP at the town’s Latham House Medical Practice, which is working with staff from other practices in the local Primary Care Network (PCN), including Syston and the Vale, to coordinate activities at the Melton centre.
Advertisement
Hide AdAdvertisement
Hide AdDr Dhanji, who has been a doctor for over 20 years and a GP for the last 12 years, talked about meeting the biggest challenge of her career and her pride at how colleagues have responded.


NICK RENNIE: What has it been like playing a vital role in such an important project as the Covid vaccination centre at the Melton Sports Village?
DR FAHREEN DHANJI: We are acutely aware of how important it is to have a vaccination centre in our community and we all feel the weight of responsibility for it being a success. There was a huge amount of planning and preparation involved in setting up the centre and with some very late evenings and early mornings we were ready for our first patients on Monday December 21. When we first opened I remember feeling very nervous and overwhelmed. This is the largest public health programme that I will ever be involved within my whole career.
NR: Being vaccinated during this pandemic has been described as quite an emotional experience for many of those people who attend. Is this something
Advertisement
Hide AdAdvertisement
Hide Adyou have observed through administering the vaccine and, if so, what kind of reactions have you had from people?


Dr FD: It certainly is an emotional experience for the patients but also the staff as well. I think it is because we are all so grateful that a vaccine has been developed so quickly and that it offers us the best opportunity to return to a life that we remember, where we can all hug our loved ones and socialise again. Although the restrictions are absolutely essential to help prevent the spread of the virus, I believe that the separation from our loved ones has been the biggest pain to bear. It’s important to remember that NHS staff are patients too and we are all desperate to see and hug our families as well, this is why we all naturally find this an emotional journey. Every patient who has attended their vaccine at our centre has been fantastic and
very kind towards all of the team involved. For some of our shielding patients, the visit to the vaccination centre was the first time they had left the house. I really feel like this is something we are all in together and I certainly get the impression from our patients that this is a beacon of hope for a brighter future.
NR: There has been a lot of praise from people about the smooth way it is organised at the Melton centre. Can you give us an insight into the roles of the
Advertisement
Hide AdAdvertisement
Hide Addifferent people, including medical staff and volunteers, and describe why it has all worked so well?
Dr FD: We have been delighted to read some of the positive comments on social media regarding the smooth running of the centre and from comments shared with our staff in person on the day. There are a huge amount of operational challenges with delivering the vaccine from a central community space and the centre could not function without GPs, nurses, healthcare assistants, first responders, IT support, cleaners, receptionists, practice managers, administration staff, stewards and volunteers. Patients will see only a handful of the staff involved in the whole process and there are almost as many people behind the scenes preparing the vaccines, regularly cleaning the centre and managing the stock and administration involved as well. Lots of our team are also made up of retired doctors and nurses who have come out of retirement to support the vaccination movement or staff are working at the centre on their days off so that we can maintain our practice operations at the same time as running the vaccinations off site. I’m immensely proud of every person involved in making it happen.
NR: It is clear that the vaccination programme across the UK has been swifter than just about anywhere else in the world. Why do you think this is the case from your experiences of working at the Melton Vaccination Centre?
Dr FD: The achievement locally has been largely down to the collaboration between the PCN, CCG and LLR Alliance and the resourcefulness of the PCNs across the UK that were instructed to develop local programmes to achieve the scale needed to provide vaccinations in their communities.
Advertisement
Hide AdAdvertisement
Hide AdOur PCN is made up of four local practices with a total patient population of 70,000. We came together at the end of November to discuss the planning for our community. Melton Mowbray was identified as the most suitable town to operate from and Melton Borough Council supported us to identify the most appropriate site that could offer the ease of access, parking and availability that we need. Hundreds of other PCNs across the UK are also delivering the same programme which is what I believe has been instrumental in the successful roll-out of the vaccinations.
The original vaccine cold store complexity meant that offering vaccines from our practices was not possible at the start but it was also necessary to identify new sites to avoid congestion at our GP premises as the infection numbers continued to rise. Patients are also aware that a group of vaccination super centres were also opened in January in city locations across the UK. These super centres have also invited people to appointments in parallel with the PCNs, supporting the goal to offer the vaccination to all patients in the JCVI top four priority groups as quickly as possible. We have found that our patients have largely chosen to receive their vaccination from our PCN centre as it offers them the convenience of staying in their local community.
NR: What has the uptake of coronavirus vaccination jabs been like locally and have you had any patients who were unsure about having one or who have
declined to have one?
Dr FD: We have experienced a really positive uptake from all patients who have been offered their vaccinations. People may decline our invitations for a number of reasons and this could include a current illness preventing them from participating at that time or because they have had the first dose vaccine at a super centre. There is a lot of really useful information available online both at our practice website and at NHS England, to help patients understand more about the vaccines available and the processes we are following to deliver them.
Advertisement
Hide AdAdvertisement
Hide AdIn addition there are also lots of helpful videos available in multi languages to support patients receiving the information they need. Patients can go to www.lhmp.co.uk/covid-19-vaccine/ to access this information and more about coronavirus.
Last weeek we had vaccinated over 12,500 patients from our PCN at the Vaccination centre in Melton Mowbray. We would really like our community to understand that the vaccination centre can only operate when we have the vaccines. The vaccination delivery from NHS England is ad-hoc and we usually receive notification of our next delivery five to seven days in advance of it arriving. Once we have confirmation of our next delivery each practice in our PCN then have to activate all of the processes involved to staff and run the centre but also to invite patients for their vaccinations. It’s a mammoth task but one that we are all achieving and I’m so proud of how everyone in Primary Care has risen to the challenge.
NR: How would you summarise the challenges of doing your job in the ongoing pandemic, in terms of dealing with patients for all the other ailments you need to treat aside from Covid?
Dr FD: The biggest challenge that I have found is that this is a completely new way of working in primary care. At the start of this in March last year it was very difficult as we were dealing with a virus that we didn’t know much about and as the situation unfolded, information for our operations changed daily and we had a real challenge to keep up. This meant that we had to join regional meetings and Covid-19 task forces to help us understand the guidance for primary care settings to be able to identify what we can do at our practice. As the situation has become more complex it remains a very challenging time for the whole NHS and sometimes I think we can all feel exhausted at the sheer scale of it. I can honestly say that I have never been busier in my entire life and I have found it tough to balance my clinical role alongside being part of the LLR Covid-19 group. My situation is not unique and I have nothing but respect and empathy for everyone who works within the healthcare sector as there won’t be a single department or role that hasn’t been impacted or challenged by the virus.
Advertisement
Hide AdAdvertisement
Hide AdWhere I am most concerned is for the patients who may be so worried about the virus that they are putting off reaching out to their GP for support. I would like to urge anyone with a health concern that is troubling them to get in touch with us. There are a number of ways patients can initiate this conversation and one fantastic tool is the online consultation programme. Through this tool a patient can write to us to explain their concerns and even attach pictures, which are reviewed by their GP. This enables your doctor to review your concerns and take the appropriate next steps. This may involve inviting patients to visit the practice and I would like to assure everyone that we have implemented robust infection prevention measures to keep everyone safe at Latham House.
NR What kind of feedback have you had from patients at the Melton Vaccination Centre and can you mention some of the nice comments you have had as people have had their jab (no names of course)?
Dr FD: We have been totally blown away with the lovely comments people have taken the time to share with us, especially on social media as this helps spread reassurance across our community. Everyone has commented on how well organised the events were and we are always delighted when people recognise the efforts of the whole team who shared their journey on the day. When we opened the centre we created a short video which we shared on social media and our website to help patients understand what to expect at their appointment and it was fantastic to know it received over 10,000 views and positive
feedback as we really wanted to help our patients feel reassured about their vaccination appointment at the community space.
Advertisement
Hide AdAdvertisement
Hide AdIt was also particularly nice to receive some lovely words of thanks from our MP, Alicia Kearns on her social media page as well. People seem to really understand the challenge involved and to share their appreciation and thanks is a huge boost to us all. Thank you to everyone who continues to show us their support. It really does mean a lot to the whole team.
NR: Can you describe what happens when someone attends the centre for their vaccination and is there anything they can do which would make your job and
those of your colleagues easier?
Dr FD: Patients will be contacted by their GP practice to invite them for their Covid-19 vaccination. We have been managing this with phone calls, letters and we are now also supporting the NHS SMS text service from Accubook, where the patient responds to a text invitation and books their appointment by following a unique link received. We are now offering the vaccine to all of our patients in the JCVI priority group 6 who have been defined by their clinical conditions. Within this priority group there are some exceptions which will have to adhere to within the programme. This is particularly the case for our asthmatic patients. Not every patient that has asthma is considered to be in the JCVI priority group 6. Only patients with asthma that requires continuous or repeated use of systemic steroids or with previous exacerbations requiring hospital admission are considered to be in this priority group and will get an invite from the practice.
We hope to be able to offer more vaccinations to the other groups as we progress. If anyone over the age of 65yrs has not yet had their vaccine then we would urge them to get in touch with us and book their appointment.
Advertisement
Hide AdAdvertisement
Hide AdEach patient will need to have two doses of the vaccine and to go to two appointments. The first dose of the vaccine should give you good protection from coronavirus. But you need to have the two doses to give you longer lasting protection.
On the day of your vaccination appointment you’ll need to bring a face covering, unless you cannot wear one for a health or disability reason. If you need a carer you can bring them with you on the day. On arrival we may ask you to wear a surgical face mask provided by the centre. This is to ensure that we are effectively managing the prevention of the virus transmittal for the benefit of all the patients and staff who attend the centre. In addition we have put in place robust measures to help keep our team and patients safe from Covid-19 and we manage regular cleaning and social distancing in waiting areas. Patients should not attend their vaccination appointment if they have symptoms or if they have had the virus in the last four weeks.
Your appointment should last for around 30 to 45 minutes. You’ll be asked some questions about your medical history. It’s important to tell the staff giving you the vaccination if you have ever had a severe allergic reaction or you are pregnant.
Once checked in you will be asked to take a seat in our sectioned out safe waiting area. You will then be called to one of the vaccination stations for your injection. We are always grateful when patients are prepared and have their clothing raised ready for their injection. However, the vaccination centre is very cold so we completely support anyone keeping their sleeves down until absolutely necessary. You will then be asked a series of check questions again and will be given an injection of the vaccine into your upper arm.
Advertisement
Hide AdAdvertisement
Hide AdAfter the vaccination you may be asked to wait for 15 minutes after having the vaccination. This is in the unlikely event you have a serious reaction to the vaccine. Research has found it’s very rare to have a serious allergic reaction to the vaccine. If this does happen, it usually happens within minutes.
The team are trained to deal with reactions and treat them immediately. You will also be given a leaflet about what to expect after your vaccination to take home with you.